Bone Cement and Joint Replacement
AskCoryC_MD : Surgeon, “Then I simply glue your knee replacement parts to the bone.”…“Uh…did you just say you use GLUE when you replace a knee joint?” – concerned future patient
First, thank you “concerned furture patient” for listening so carefully to my description of your upcoming knee replacement. And yes, I often times use “glue” (really more commonly called “cement”) during the knee replacement surgery to fix the parts to your bone.
Let me explain. A knee replacement is really just a RESURFACING of) the end of the femur (thigh bone), b) the top of the tibia (shin bone) and c) the undersurface of the patella (knee cap). Contrary to popular perception, we remove just a thin layer of bone, leaving the rest of the bone and ligaments around the knee undisturbed.
Check out the picture below. See the “cut” ends of the femur and tibia. See the two thin pieces of metal (one for the femur, one for the tibia) that replaces the removed bone.
We use a plastic piece (okay, medical grade polyethylene) to take the place of the removed bone from the underside of the patella so no bone touches the artificial metal parts. Notice the plastic piece that goes in between the femur and tibia – this is essentially a new cartilage surface for the knee joint.
So…back to the cement. Technically speaking, bone cement is defined as a family of materials that consist of a powder phase and a liquid phase which, after mixing, form a plastic paste which has the ability to self-set once implanted in the body. With knee replacement we "fix" the two metal pieces (and the plastic piece behind the patella) into the prepared bone surface using bone cement.
Bone cement is generally mixed in the operating room on an ‘as needed’ basis. Because the curing time is fast, the bone cement is usually not prepared until the whole surgery needed to permanently place a component of an artificial joint has been completed. The cement starts in a powder form and is mixed with a specific liquid (called monomer). The cement is usually mixed in a negative vacuum bowl designed to reduce the porosity (remove the air bubbles). This makes a cake icing-like material that we coat the bone and artificial parts with, then hold them in place. In the matter of just a few minutes, that bone cement hardens and the artificial parts are locked solidly to the bone.
Once the cement has cured, its job is primarily structural – to hold the device in place permanently and facilitate load transfer from the device into the remaining bone. This is one of the reasons patients can get up and walk immediately after surgery. The parts are stable and recovery begins right away.
What Is Bone Cement Made Of?
Today, polymethylmethacrylate (PMMA) is the most widely used bone cement used for implant fixation. PMMA as a polymer is commonly used in daily life. Plexiglas (which has emerged as a high-demand commodity during the COVID-19 pandemic), is an acrylic resin that was invented at the beginning of the 20th century and, at that time, manufactured under complex technical conditions. In 1936, cold curing of methylmethacrylate (MMA) was developed and the product was introduced into dentistry and craniofacial surgery. Sir John Charnley, considered a pioneer of modern artificial joint replacement, developed the science and art of modern cementing technique in his laboratories in the late 1950s. While methods have been improved and modified, cement fixation remains the gold standard, against which all forms of implant fixation techniques are assessed.
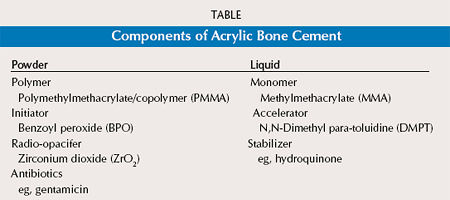
Additional Bone Cement Facts
Bone cement has a characteristic fume-like odor similar to a dry erase marker.
The powder mainly consists of bead-shaped particles with a diameter of approximately 40 microns. These particles contain PMMA and/or methyl methacrylate copolymers, and one of three activators of the polymerization process. [benzoyl peroxide (BPO) (so called initiator), zirconia (ZrO2), or barium sulphate (BaSO4) to provide radiodensity, and sometimes an antibiotic].
The liquid component mainly contains the monomer MMA but also the second activator of the polymerization process, N,N-Dimethyl para-toluidine (DMPT) (so called accelerator), and hydroquinone as a stabilizer to prevent self-curing of the monomer in the liquid during storage.
Temperature and humidity influencing the curing-rate of the cement. Bone cement starts as a powder and a liquid, mixes to a cake icing consistency, then progresses to a playdough-like consistency. It eventually hardens to a stone-like consistency.
In addition to the strong odor, the curing process is an exothermic reaction and releases a lot of heat during mixing. The application process is similar to icing a cake (with hot, smelly icing).
Alternative antibiotic and antiseptic agents will continue to be trialed by manufacturers in the future. The future will likely also see more sophisticated technical assistance to guide the timing of insertion of the cement, but no technology will replace knowledge and experience. Education and training will remain the cornerstone for optimized cement handling and application
Cemented vs. Cementless Joint Implants
Bone Cement is not used for every knee replacement. While cement is often used and is particularly useful with thinning bone, some patients will benefit from cementLESS knee replacements to improve long-term success (20 years and beyond). Artificial joints may rely solely on bone ingrowth (cementless), may have some components cemented and others that are fixed by ingrowth, or may be completely cemented. The fixation method(s) used often depend on the health of the patient's bones, the type of device implanted, and the surgeon's background and preferences. The key is to optimize outcomes by individualizing each knee replacement.