Is Robotic-Assisted Joint Replacement Right for You?
Advanced robotic technology has transformed joint replacement surgery in Middle Tennessee, offering patients in Nashville, Franklin, and Brentwood unprecedented precision and improved outcomes. As a fellowship-trained orthopedic surgeon and Mako robotic specialist, Dr. Cory Calendine uses cutting-edge robotic-assisted technology to deliver personalized hip and knee replacements that are tailored to your unique anatomy.
If you're already a candidate for joint replacement surgery, robotic-assisted surgery can significantly enhance your results. The Mako robotic system creates a personalized 3D model of your joint using CT imaging, allowing Dr. Calendine to plan your exact procedure before you even enter the operating room. This advanced planning typically results in better implant positioning, preserved healthy bone and tissue, and faster recovery times for patients throughout the Greater Nashville area.
Dr. Calendine currently performs Mako robotic-assisted surgery for partial knee replacements, total knee replacements, and total hip replacements at Williamson Medical Center, making him one of the region's most experienced robotic joint replacement specialists.
How robotic-assisted surgery works
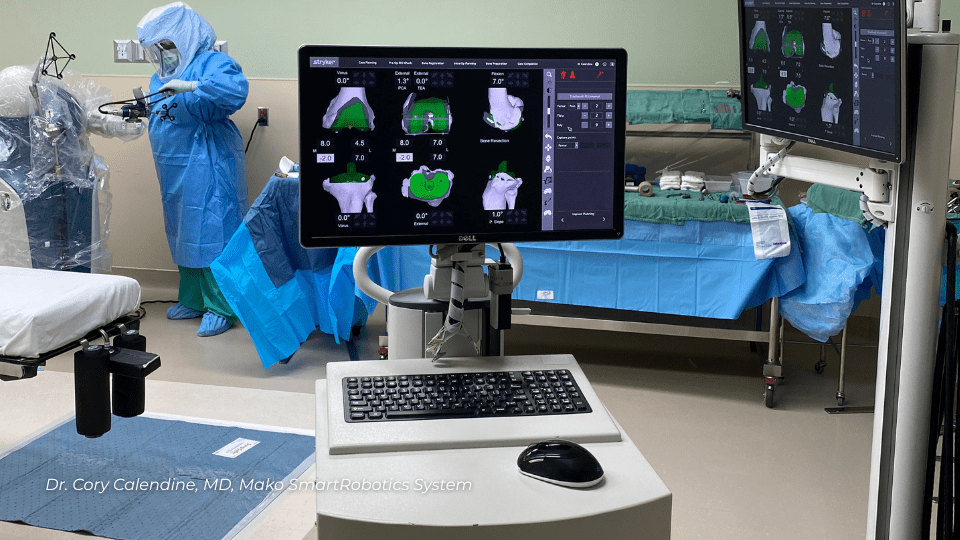
Before your robotic hip replacement surgery at Williamson Medical Center, Dr. Calendine orders a specialized CT scan that creates a detailed 3D virtual model of your unique hip anatomy. This advanced imaging provides critical information that traditional X-rays cannot reveal, allowing Dr. Calendine to precisely plan your implant size, placement, and positioning for optimal long-term results.
During your Mako robotic-assisted total hip replacement, Dr. Calendine maintains complete control while the robotic arm enhances his surgical precision. The Mako system provides continuous real-time feedback throughout your procedure, enabling Dr. Calendine to monitor joint movement and tension while making adjustments to your surgical plan as needed. This level of precision is what sets robotic joint replacement apart from traditional hip surgery techniques.
In the operating room, Dr. Calendine guides the Mako robotic arm to remove only the damaged arthritic bone and cartilage from your hip joint. The system's virtual boundary technology provides tactile feedback that helps ensure he stays within the pre-planned surgical boundaries, preserving your healthy bone and tissue. When placing your new hip implant, the robotic arm assists Dr. Calendine in achieving the exact angle and position determined in your personalized surgical plan, resulting in superior implant alignment and improved joint function for Nashville-area patients.

If you’re one of the millions of Americans suffering from pain caused by arthritis or an injury to the hip or knee, and you haven’t experienced adequate relief with conservative treatment options, Mako Robotic-Arm Assisted Surgery might be right for you. Source: https://patients.stryker.com/hip-replacement/options/mako-robotic-arm-assisted
advantages of robotic-assisted joint replacement
Dr. Calendine's expertise with Mako robotic-assisted surgery offers Nashville and Franklin patients significant advantages over traditional joint replacement procedures. By utilizing advanced robotic technology at Williamson Medical Center, Dr. Calendine can customize each hip and knee replacement surgery to match your individual anatomy, soft tissue structure, and lifestyle needs. This personalized approach to robotic joint replacement surgery has helped countless Middle Tennessee patients return to their active lifestyles faster and with better long-term outcomes.(Source:
https://patients.stryker.com/hip-replacement/options/mako-robotic-arm-assisted)
The precision of Dr. Calendine's robotic-assisted joint replacement technique delivers measurable improvements for patients throughout the Greater Nashville area. Enhanced accuracy through more precise implant positioning creates a more natural-feeling joint after surgery, while improved safety protocols reduce the risk of injury to surrounding healthy tissues and muscles. The minimally invasive nature of Mako robotic surgery requires only smaller incisions that promote faster healing and less scarring, leading to accelerated rehabilitation timelines compared to traditional joint replacement surgery. Patients consistently experience superior long-term function with better joint stability and range of motion for years to come.
Mako robotic-assisted surgery has demonstrated superior outcomes in multiple clinical studies that directly benefit Dr. Calendine's patients in Nashville and Franklin. Better implant alignment ensures more accurate placement according to each patient's personalized surgical plan, while reduced complications mean a lower risk of hip dislocation and implant loosening. The advanced robotic technology results in less blood loss during surgery, minimizing surgical trauma and making recovery easier for patients. The system's precision allows for improved replication of your original joint mechanics, creating a more natural joint feel, while maximizing preservation of healthy bone and cartilage tissue throughout the procedure.
As one of Middle Tennessee's most experienced Mako robotic surgeons, Dr. Calendine combines cutting-edge technology with fellowship-trained expertise to deliver the best possible outcomes for joint replacement patients in Nashville, Franklin, and surrounding communities. His extensive experience with the Mako robotic system ensures that patients receive the most advanced joint replacement care available in the region, with personalized treatment plans designed to restore mobility and improve quality of life for years to come.
Is Mako Robotic Joint replacement an option for me?
If you're experiencing severe joint pain or stiffness that's impacting your daily life, Mako robotic-assisted joint replacement with Dr. Calendine may be the solution you've been seeking. This advanced surgical option is ideal for patients dealing with osteoarthritis, rheumatoid arthritis, traumatic arthritis, or avascular necrosis who haven't found adequate relief through conservative treatments such as physical therapy, medications, injections, or bracing. Dr. Calendine evaluates each patient's unique situation at Williamson Medical Center to determine if they're a candidate for this cutting-edge robotic joint replacement technology.
Many Nashville and Franklin patients who have tried multiple non-surgical treatments without success discover that Mako robotic surgery offers them a path back to an active, pain-free lifestyle. As a fellowship-trained orthopedic surgeon specializing in robotic joint replacement, Dr. Calendine has helped hundreds of Middle Tennessee residents overcome chronic joint pain and return to the activities they love. If traditional treatments haven't provided the relief you need, scheduling a consultation to discuss whether Mako robotic-assisted hip or knee replacement is right for you could be the first step toward reclaiming your mobility and quality of life.
mako robotic total hip replacement by stryker
Your Mako robotic joint replacement surgery with Dr. Calendine typically takes less than an hour, during which he'll carefully remove the damaged parts of your joint and place your new implant with precision that only robotic technology can provide. The recovery process at Williamson Medical Center is designed around your comfort and safety. You'll spend a few hours in our recovery area while the anesthesia wears off, and our nursing team will closely monitor your progress every step of the way.
Most patients return home the same day after their robotic joint replacement surgery, though your exact length of stay depends on how quickly you're moving around and feeling comfortable. Dr. Calendine and his team consider your overall health, age, and how active you were before surgery when creating your personalized recovery plan. Before you head home to begin the next phase of your healing journey, our orthopedic team will make sure you have everything you need for a safe and successful recovery, including detailed instructions, follow-up appointments, and any necessary equipment or support services.
joint replacement recovery
Your successful recovery from Mako robotic joint replacement surgery starts with following Dr. Calendine's personalized post-operative instructions during your first few weeks at home. The precision of robotic surgery typically means smaller incisions and faster healing, though proper wound care remains essential for optimal results. Dr. Calendine will remove your stitches or staples about two weeks after surgery, and until then, keep your incision dry and protected with bandages to prevent irritation from clothing.
Many Nashville and Franklin patients experience some appetite changes during the first few weeks after their robotic joint replacement surgery, which is completely normal. Dr. Calendine's team will provide you with nutrition guidelines that often include a balanced diet with iron supplements to support tissue healing and rebuild your strength. Staying well-hydrated also plays a crucial role in your recovery process.
The excellent outcomes that Dr. Calendine achieves with Mako robotic surgery mean most patients return to their daily activities within six weeks of their procedure. By three months after your robotic joint replacement at Williamson Medical Center, you'll likely have regained the strength and endurance you had before joint pain limited your activities. While you'll be able to enjoy most of your favorite activities without restrictions, Dr. Calendine will guide you optimizing your post-surgery activity to ensure your new joint lasts for decades to come.
Your timeline for returning to driving and work depends on several factors that Dr. Calendine will discuss with you personally. Most patients can drive again at four to six weeks after surgery, though this may be sooner if your left leg was operated on. For your safety, Dr. Calendine will want to ensure you're no longer taking pain medications and that your reaction time has fully returned before getting behind the wheel. If you work at a desk job, you can typically return to work within four to six weeks of your robotic joint replacement surgery. Those with more physically demanding careers may need up to three months to fully recover, though Dr. Calendine will work with you to determine the best timeline based on your specific job requirements and healing progress. Throughout your recovery, Dr. Calendine and his team will monitor your progress and adjust your rehabilitation plan to help you achieve the best possible outcome from your robotic joint replacement surgery.
Source:
American Academy of Orthopaedic Surgeons, https://orthoinfo.aaos.org/; American Association of Hip and Knee Surgeons, https://hipknee.aahks.org/total-hip-replacement/; Cleveland Clinic Foundation, https://health.clevelandclinic.org/; Stryker, https://patients.stryker.com/hip-replacement/options/mako-robotic-arm-assistedCory Calendine, MD is an Orthopedic Surgeon and founding partner of the Bone and Joint Institute of Tennessee at Williamson County Hospital in Franklin, TN. Dr. Calendine is an expert in Joint Replacement, specializing in Hip and Knee Surgery. From diagnosis through treatment, the Orthopedic Surgical experts at the Bone and Joint Institute use the latest techniques and technology to improve care for people with musculoskeletal problems. For more information, please contact our office or schedule your appointment today.


